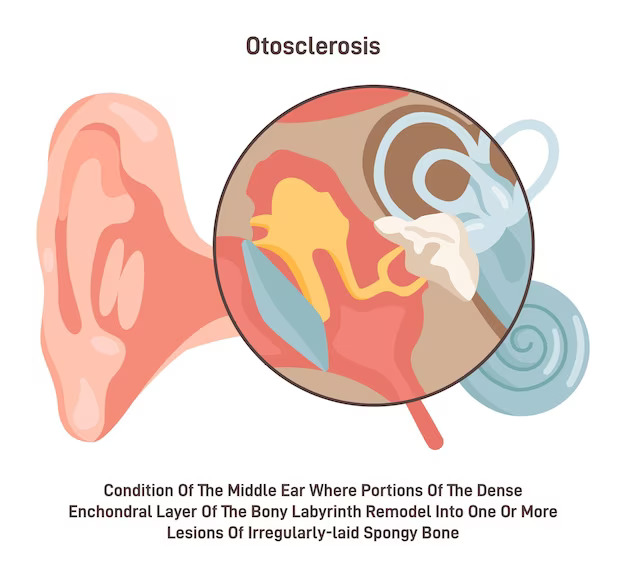
Otosclerosis is a common cause of progressive hearing loss, especially in adults. It refers to an abnormal growth of bone in the middle ear, and more specifically around the stapes bone, which is the smallest bone in the body. This abnormal growth prevents the stapes from vibrating in response to sound waves, leading to a type of hearing loss called conductive hearing loss. In some cases, otosclerosis can also affect the inner ear, leading to sensorineural hearing loss or a combination of both types of hearing loss.
Epidemiology and Pathophysiology of Otosclerosis.
Otosclerosis tends to occur more frequently in women than men and is most diagnosed in people between the ages of 20 and 50. Its prevalence differs across ethnic groups. It is most common in Caucasians, followed by Hispanics, Asians, and is least common among African-Americans.
The exact cause of otosclerosis is still unknown, but it is believed to result from a combination of genetic and environmental factors. Histopathologically, it’s characterized by an initial active phase (otospongiosis), in which the normal endochondral bone layer of the otic capsule is replaced by vascular connective tissue. Later, this tissue undergoes gradual transformation into mature, sclerotic bone (otosclerosis), which can compromise the mobility of the stapes and other structures in the middle and inner ear.
How Do We Hear?
Understanding otosclerosis requires some knowledge of how we hear. Sound waves enter the outer ear and travel to the middle ear, where they cause vibration of the eardrum and the attached ossicles: malleus, incus, and stapes. The vibrating stapes pushes into the oval window of the cochlea, a spiral-shaped bone in the inner ear filled with fluid and lined with hair cells.
When the stapes pushes into the oval window, it sets off a wave in the cochlear fluid, causing the hair cells to move. This movement of hair cells generates electrical signals which are sent to the brain via the auditory nerve. The brain interprets these signals as sound.
What Causes Otosclerosis?
The exact cause of otosclerosis remains unknown. However, research suggests a combination of genetic predisposition and environmental factors such as viral infections (specifically measles) and hormonal influences. For instance, it often worsens during pregnancy, which suggests a role of hormones in the disease process.
Symptoms of Otosclerosis
The primary symptom of otosclerosis is a progressive hearing loss, which initially affects the ability to hear low-pitched sounds or whispers. Other symptoms may include tinnitus (a ringing or buzzing sound in the ear), vertigo or imbalance, though these symptoms are less common.
Otosclerosis primarily affects an individual’s hearing capability and presents with signs and symptoms centered around this key function. The impact of hearing loss from otosclerosis varies and often depends on the disease’s severity, individual tolerance, and the specific scenarios or environments the person encounters in daily life. Here are some situations to consider:
-
Communication: One of the most immediate impacts of otosclerosis is on personal communication. Patients may often find themselves asking others to repeat what they’ve said, or they may misunderstand conversations, especially in noisy environments. In social situations, they might feel isolated or disconnected because of the difficulty in following group conversations.
-
Professional scenarios: In a work setting, this can affect performance and engagement, particularly in jobs that require accurate communication. It may be challenging to follow meetings, discussions, or phone conversations.
-
Safety: Safety can also be a concern, especially when the hearing loss is significant. For example, individuals may not hear alarms, warning shouts, approaching vehicles, or the ringing of a telephone or doorbell.
-
Tinnitus and vertigo: In addition to hearing loss, patients with otosclerosis may also experience tinnitus – a constant ringing or buzzing noise in the ears. This can be particularly bothersome during quiet times, such as when trying to sleep or concentrate on a task. Some patients may also experience balance issues or vertigo, though these symptoms are less common.
-
Impact on enjoyment of activities: Leisure activities that were once enjoyed may become frustrating or less fulfilling. This can include watching TV, listening to music, attending concerts or sports events, or even simply enjoying nature. For example, a patient might find it difficult to follow dialogue in movies or TV shows, or struggle to hear the melody or lyrics in music.
-
Emotional impact: The cumulative effect of these symptoms can lead to emotional distress. Patients may experience frustration, embarrassment, or a feeling of isolation due to their hearing difficulties. There can also be a significant impact on self-esteem and confidence, potentially leading to withdrawal from social situations and even depression in some cases.
Remember, these signs and symptoms can vary from person to person. It’s also important to note that these symptoms are common to many types of hearing loss and not exclusive to otosclerosis. Therefore, if these symptoms are present, it’s crucial to consult with a healthcare provider for an accurate diagnosis and appropriate treatment.
Stages of Otosclerosis
Otosclerosis is typically categorized by the area of the ear it affects and its progression. It’s important to note that the clinical progression of otosclerosis may not align perfectly with the histological stages due to variability in symptom presentation and disease progression among individuals. The following represents the generally accepted stages and types of otosclerosis:
-
Histologic Otosclerosis (Fenestral Phase): This stage may not present any noticeable symptoms and is detectable only through histological examination of temporal bone specimens. Here, otosclerotic lesions affect the bony labyrinth of the ear, particularly the area around the oval window (fenestra ovalis), hence the name “fenestral phase”.
-
Clinical Otosclerosis (Cochlear Phase): As the disease progresses, patients begin to experience symptoms, mainly conductive hearing loss. This progression marks the transition to clinical otosclerosis, also known as the “cochlear phase”. The otosclerotic bone starts to encase the stapes bone in the middle ear, inhibiting its movement and thereby disrupting the transmission of sound waves from the middle ear to the inner ear.
-
Late-stage Otosclerosis: In some cases, the otosclerotic bone can infiltrate the inner ear (cochlear otosclerosis), leading to sensorineural hearing loss. Patients can end up with mixed hearing loss (both conductive and sensorineural) in these situations.




1 Comment
Just wish to ѕay your article is as amazing.
The clarity in your post is simply cool and
i coulԁ assume you’re an expert on this subject.
Wеll with your permission allow me to grab your feed to kеep
updated witһ forthcoming poѕt. Thanks a million and please continue the enjoyable work.
Comments are closed for this article!